Burns Treatment in Perumbakam
Your Trusted Partner in Burns
Burns are tissue damage brought on by heat, chemicals, electricity, radiation or the sun. We are here to provide you with top-notch care and guidance to tackle your problems.
Understanding Burns Treatment
WHAT IS BURN?
A burn occurs when heat, chemicals, sunlight, electricity or radiation damages skin tissue. Most burns happen accidentally. There are different degrees of burns. Your healthcare provider determines the seriousness (degree) of a burn based on the depth of the burn and the amount of affected skin. Burns can be painful. Left untreated, a burn can lead to infection.
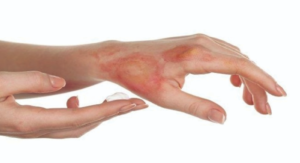
Symptoms
- Chemicals, such as cement, acids or drain cleaners
- Radiation.
- Electricity.
- Sun (ultraviolet or UV light).
- Redness
- Nightmares
- Swelling
- Peeling or Sloughing
Healthcare providers classify burns by degrees of severity. Your provider will evaluate the extent of skin damage. Burn degrees include:
- First-degree burns are mild (like most sunburns). The top layer of skin (epidermis) turns red and is painful but doesn’t typically blister.
- Second-degree burns affect skin’s top and lower layers (dermis). You may experience pain, redness, swelling and blistering.
- Third-degree burns affect all three skin layers: epidermis, dermis and fat. The burn also destroys hair follicles and sweat glands. Because third-degree burns damage nerve endings, you probably won’t feel pain in the area of the burn itself, rather adjacent to it. Burned skin may be black, white or red with a leathery appearance.
What are the types of burns?
Causes
Burns are caused by:
- Fire
- Hot liquid or steam
- Hot metal, glass or other objects
- Electrical currents
- Radiation, such as that from X-rays
- Sunlight or other sources of ultraviolet radiation, such as a tanning bed
- Chemicals such as strong acids, lye, paint thinner or gasoline
- Abuse
Complications
Complications of deep or widespread burns can include:
- Bacterial infection, which may lead to a bloodstream infection (sepsis)
- Fluid loss, including low blood volume (hypovolemia)
- Dangerously low body temperature (hypothermia)
- Breathing problems from the intake of hot air or smoke
- Scars or ridged areas caused by an overgrowth of scar tissue (keloids)
- Bone and joint problems, such as when scar tissue causes the shortening and tightening of skin, muscles or tendons (contractures)
Prevention
To reduce the risk of common household burns:
- Never leave items cooking on the stove unattended.
- Turn pot handles toward the rear of the stove.
- Don’t carry or hold a child while cooking at the stove.
- Keep hot liquids out of the reach of children and pets.
- Keep electrical appliances away from water.
- Check the temperature of food before serving it to a child. Don’t heat a baby’s bottle in the microwave.
- Never cook while wearing loose fitting clothes that could catch fire over the stove.
Diagnosis
If you go to a doctor for burn treatment, he or she will assess the severity of your burn by examining your skin. He or she may recommend that you be transferred to a burn center if your burn covers more than 10 percent of your total body surface area, is very deep, is on the face, feet or groin, or meets other criteria established by the American Burn Association.
Your doctor will check for other injuries and might order lab tests, X-rays or other diagnostic procedures.
Medical treatment
Water-based treatments:
Your care team may use techniques such as ultrasound mist therapy to clean and stimulate the wound tissue.
Fluids to prevent dehydration:
You may need intravenous (IV) fluids to prevent dehydration and organ failure
Pain and anxiety medications:
Healing burns can be incredibly painful. You may need morphine and anti-anxiety medications — particularly for dressing changes.
Burn creams and ointments:
If you are not being transferred to a burn center, your care team may select from a variety of topical products for wound healing, such as bacitracin and silver sulfadiazine (Silvadene). These help prevent infection and prepare the wound to close.
Dressings:
Your care team may also use various specialty wound dressings to prepare the wound to heal. If you are being transferred to a burn center, your wound will likely be covered in dry gauze only.
Drugs that fight infection:
If you develop an infection, you may need IV antibiotics.
Lifestyle and home remedies
To treat minor burns, follow these steps:
- Cool the burn: Hold the burned area under cool (not cold) running water or apply a cool, wet compress until the pain eases. Don’t use ice. Putting ice directly on a burn can cause further damage to the tissue.
- Remove rings or other tight items: Try to do this quickly and gently, before the burned area swells.
- Don’t break blisters: Fluid-filled blisters protect against infection. If a blister breaks, clean the area with water (mild soap is optional). Apply an antibiotic ointment. But if a rash appears, stop using the ointment.
- Apply lotion: Once a burn is completely cooled, apply a lotion, such as one that contains aloe vera or a moisturizer. This helps prevent drying and provides relief.
- Bandage the burn: Cover the burn with a sterile gauze bandage (not fluffy cotton). Wrap it loosely to avoid putting pressure on burned skin. Bandaging keeps air off the area, reduces pain and protects blistered skin.
- Take a pain reliever: Over-the-counter medications, such as ibuprofen (Advil, Motrin IB, others), naproxen sodium (Aleve) or acetaminophen (Tylenol, others), can help relieve pain.
- Consider a tetanus shot: Make sure that your tetanus booster is up to date. Doctors recommend that people get a tetanus shot at least every 10 years.
Whether your burn was minor or serious, use sunscreen and moisturizer regularly once the wound is healed.
Frequently Asked Question on Burns
- First-degree burns: affect only the outer layer of the skin (epidermis) and cause redness, pain, and swelling.
- Second-degree burns: affect the outer layer of the skin and part of the underlying layer (dermis) and may cause blistering, intense pain, and swelling.
- Third-degree burns: extend through the entire thickness of the skin and may damage underlying tissues, nerves, and blood vessels, leading to numbness or difficulty moving the affected area.
- Clean the burn gently with mild soap and water.
- Apply aloe vera gel or an antibiotic ointment to promote healing and prevent infection.
- Cover the burn with a sterile, non-adhesive dressing.
- Take over-the-counter pain relievers as needed.
- Avoid popping blisters, as this can increase the risk of infection.
- Seek immediate medical attention if the burn is severe, covers a large area of the body, or involves the face, hands, feet, groin, or major joints.
- Seek medical attention if the burn shows signs of infection, such as increased pain, redness, swelling, warmth, or drainage of pus.
For minor burns:
- Cool the burn with cool running water for several minutes to reduce pain and swelling.
- Cover the burn with a sterile, non-adhesive dressing.
- Take over-the-counter pain relievers as needed.
- For severe burns or burns with blistering, seek immediate medical attention.
